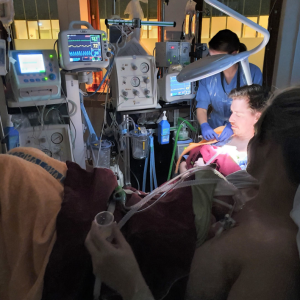
© Stina Klemming
As preterm newborns and mothers have different medical needs, they are usually treated on different wards. However, the concept of mother-newborn coupled care breaks with that tradition and instead keeps them together throughout their hospitalization. This allows for immediate skin-to-skin contact after birth, a higher quality of care, and lower rates of morbidity and mortality for the infant. The concept is already well-established in Swedish and Finish maternity hospitals and serves as a model for the implementation of couplet care in other countries. The 10th edition of the recommended standards for newborn ICU design examines how couplet care can be implemented, what requirements are necessary and the benefits for staff and patients.
From the moment of birth onward, a newborn needs to be nurtured, loved, and cared for by its parents. However, separation of mother and infant after birth is still common, especially for preterm and sick infants. Yet only by treating them together, it can be assured that immediate skin-to-skin contact is possible. Mother-Newborn Couplet Care is a concept that focuses on joint care of mother and infant and provides medical care for both in one unit. This concept is strongly promoted in the new edition of the Recommended Standards for Newborn ICU Design. The 10th edition promotes the shift towards a more infant- and family-centred approach to newborn care.
The concept of couplet care was introduced in Sweden around 20 years ago and has since proved its effectiveness. Today, 16 out of 38 Swedish units and 18 out of 23 Finish maternity hospitals offer couplet care. The benefits are improved quality of care, reduced morbidity and mortality, better long-term outcomes, higher care satisfaction and well-being for parents and infants. In addition, it saves costs through higher efficiency of care, reduced resources and time, and reduced healthcare costs while promoteing the collaboration between different departments.
However, some changes are needed in order to implement couplet care successfully. The article by Klemming et al. therefore analysed the Nordic experience to serve as a model for future implementation in other regions and hospitals.
Implementing couplet care is a step-by-step process involving many actors
A strong commitment from leadership and staff is the basis for successfully implementing couplet care. As the concept requires both personnel from neonatal and obestetric departments and midwives to work together, collaboration is crucial. This offers the opportunity to create a leadership steering group with representatives from all departments involved, which has a strong decision-making mandate. They will have to decide on adjustments of the physical design of the units, dividing responsibilities and exchanging knowledge, as well as the training of healthcare professionals. Experience from Sweden and Finland shows that trainings, simulations, and visits to hospitals that have already implemented couplet care were most successful.
There are four different unit designs to facilitate couplet care
Once the new system is implemented, it can work in different ways.
- The most common implementation works regardless of where the mother and newborn are located in the hospital. Mobile obstetrics and neonatal teams provide the care for mother and child. This model requires less cross-training of staff but high mobility of teams.
- A second option is to establish a combined nursing team. The midwives are deployed at the neonatal unit and work closely with the obstetrics department. In this approach, midwives must be specially cross-trained to be able to care for both mother and newborn.
- The third option is usually applied for infants with mild medical needs such as late preterm infants. They can stay with their mother while doctors from the neonatal unit are doing daily check-ups on the newborn. The nurses need special training; however, the model is easy to apply.
- If there is the possibility to start a new department, it is advised to employ both neonatal and obstetric staff in a new perinatology unit. This increases collaboration between various medical staff, requiring less cross-training.
One example of successfully implementing couplet care, can be seen on the cover picture. It shows a mother and father in a birth room, where each is providing immediate skin-to-skin care for one of their very preterm twins. A mobile neonatal team with equipment for neonatal stabilisation is present to support.
All these models enable immediate skin-to-skin contact after birth to keep mother and child together irrespective of their clinical conditions, thus making couplet care available to preterm infants. The vision is that couplet care will be offered in every mother-newborn dyad with preterm infants to improve their survival, growth, health, and development.
Paper available at: https://www.nature.com/articles/s41372-023-01812-3
Full list of authors: Stina Klemming, Siri Lilliesköld, Sofia Arwehed, Wibke Jonas, Liisa Lehtonen, Björn Westrup
DOI: https://doi.org/10.1038/s41372-023-01812-3
Learn more about the practice and benefits of skin-to-skin contact as part of Kangaroo Mother Care.

